BACKGROUND
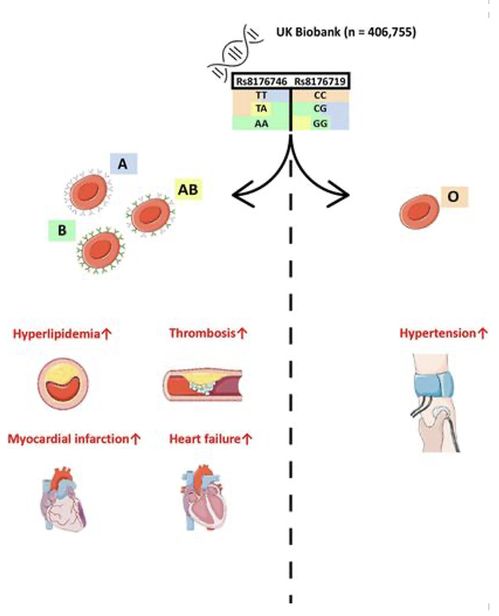
- ABO carbohydrate moieties have been labeled as a predisposition for certain viral infections, including hepatitis B, SARS-CoV-1, and recently, the novel coronavirus SARS-CoV-2
- In addition, non-O blood types, as shown here, have previously been linked to increased risk for certain health conditions, including thrombosis, a prevalent clinical characteristic of the novel coronavirus
- As COVID-19 has developed into a global pandemic, it is important to determine whether ABO blood group types and the associated Rh factor are linked to increased severity of COVID-19 disease, defined by both thrombosis and mortality
AIM/OBJECTIVE
To investigate a potential relationship between blood type and COVID-19 disease severity, characterized by thrombosis and mortality
To investigate a potential relationship between blood type and COVID-19 disease severity, characterized by thrombosis and mortality
METHODOLOGY
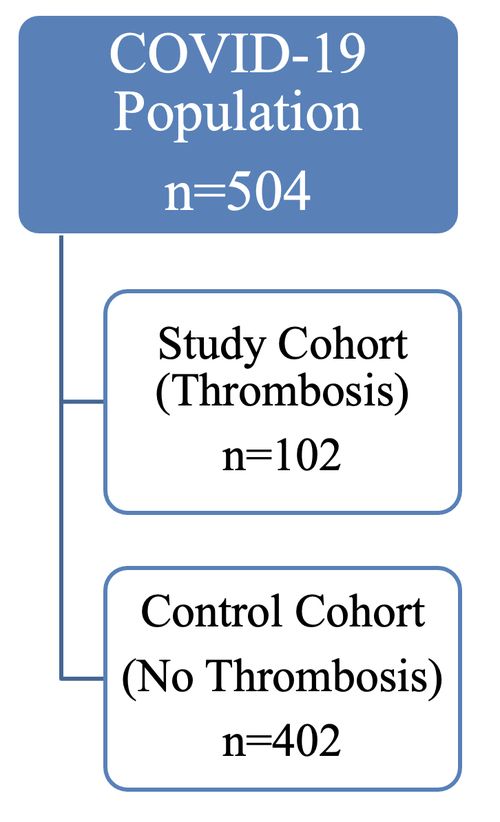
- This study included 504 total patients who tested positive for COVID-19 between March 1, 2020 and June 26, 2020 at our institution
- 102 patients had a thromboembolic event
– venous thromboembolism (VTE), pulmonary embolism (PE), arterial embolism (AE), cerebellar infarction (CI) and/or cerebral stroke (CS), and these 102 were part of the study cohort - The other 402 exhibited no signs of thromboembolic events and were denoted as the control cohort
- Pearson’s chi-squared test of homogeneity and Fisher’s exact test were utilized to compare the blood type distributions of the study cohort to the control cohort
- Incidence of individual thrombotic events was also analyzed
- A logistic regression model was conducted to control for the possible confounding effect of race, sex, and age on incidence of thrombosis and mortality
RESULTS
- There was no significant difference in incidence of thrombosis between blood types (p=0.6513)
- When stratifying by Rh factor, there was still no significant difference in incidence of thrombosis (p=0.9054)
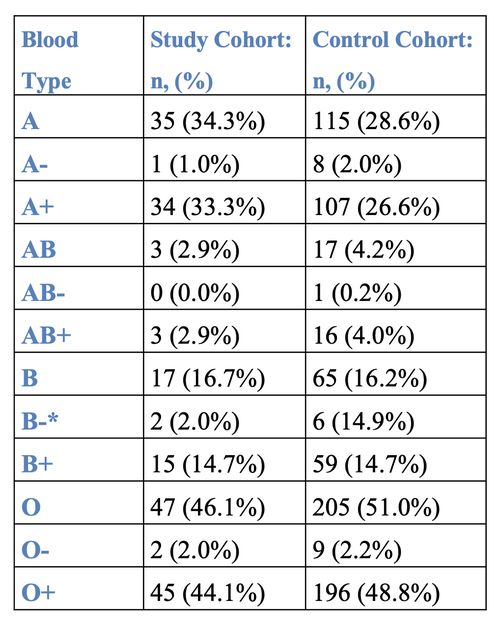
- Table 1 (shown to the left) contains a retrospective comparison of the study cohort (COVID-19+ with thrombosis) and control cohort (COVID-19+ without thrombosis) stratified according to the ABO system and Rh factor.
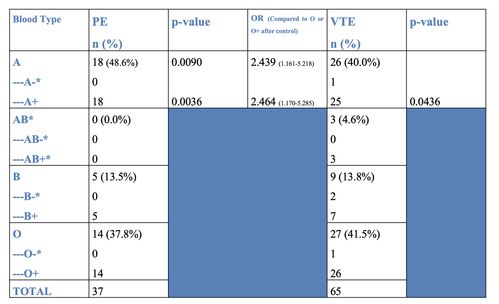
- A series of chi-squared tests and Fisher’s exact tests comparing specific thrombotic events between blood types yielded a statistically significant difference in PE incidence for blood types A and A+ and in VTE incidence for blood type A+
- After controlling for race, sex, and age, blood type A was determined to be 243.9% more likely to develop COVID-19 associated PE than blood type O
- Blood type A positive was 246.4% more likely to develop COVID-19 associated PE than blood type O positive after controlling for confounders
- After controlling for confounders, blood type A+ was no longer found to be a significant predictor for VTE compared to blood type O
- Table 2 (shown below) contains the incidence of PE and VTE in different blood types
CONCLUSION
- This study found no increased prevalence of one blood type over another between COVID-19+ patients with thrombosis compared to COVID-19+ patients without thrombosis
- This finding indicates that patients are not at higher risk for thrombosis in general from COVID-19 infection based on blood type
- When further stratifying with Rh factor, there was also no difference in prevalence of thrombosis based on blood types, demonstrating that Rh negativity and positivity does not have an effect on the correlation between blood type and COVID-19 associated thrombosis
- However, blood type A and A+ individuals were at an increased risk of developing PE, a specific thrombotic event, as compared to blood type O and O+, respectively, even after controlling for confounding variables
- In addition, type A+ blood individuals were also more likely to develop VTE than blood type O individuals, but this conclusion did not hold true after controlling for race, sex, and age
DISCUSSION
- While the findings in regards to PE and VTE show that A and A+ blood type may predispose a patient to COVID-19 associated thromboembolic events, this study was a single-center retrospective study with a small sample size
- Since the sample size was small, a type II error may have occurred
- Severity of disease may have also skewed blood typing data, as patients who were less severely affected by COVID-19 were unlikely to require blood transfusion and hence blood typing
- It is also known that individuals with blood type O generally have decreased levels of VWF. Thus, investigating the relationship between VWF level and severity of COVID-19 through prospective studies may bring more insight into COVID-19 associated coagulopathy
The data in this poster was presented at ASH Meeting 2020. Published with permission from the Copyright owner.
REFERENCES
- Johns Hopkins Coronavirus Resource Center. (2020). Johns Hopkins Coronavirus Resource Center. https://coronavirus.jhu.edu/map.html
- Zahra, K. F., Mestaghanmi, H., Jabari, M., Labriji, A., Amrani, S., & Dibane, A. (2019). Relationship study between blood groups, rhesus factor and the risk of diabetes type 2 in a population of the Sidi Othmane district, Casablanca. Endocrine Abstracts. https://doi.org/10.1530/endoabs.63.p157
- Groot, H. E., Villegas Sierra, L. E., Said, M. A., Lipsic, E., Karper, J. C., & van der Harst, P. (2020). Genetically Determined ABO Blood Group and its Associations With Health and Disease. Arteriosclerosis, Thrombosis, and Vascular Biology, 40(3), 830–838. https://doi.org/10.1161/atvbaha.119.313658
- Zietz, M., & Tatonetti, N. P. (2020). Testing the association between blood type and COVID-19 infection, intubation, and death. https://doi.org/10.1101/2020.04.08.20058073
